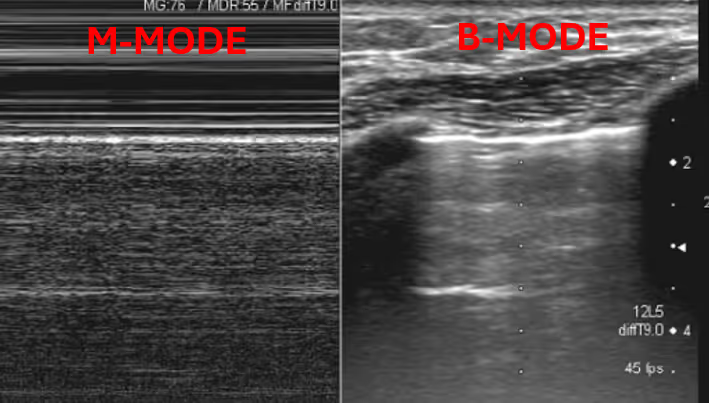
Lung ultrasound has revolutionized respiratory assessments in modern medicine, offering real-time, non-invasive, and radiation-free insights into lung conditions. It uses sound waves to create images that reflect lung pathology and its simplicity, portability and rapid applicability make it an indispensable tool for clinicians. These features also make it highly effective in reducing the need for bedside chest X-rays and CT scans.
The early days
In 1917, French physicist Paul Langevin pioneered the use of the piezoelectric properties of quartz to successfully receive and transmit ultrasound waves. His work led to the proliferation of ultrasound during World War I, where ultrasound was used to detect enemy submarines. Subsequently Karl and Friederich Dussik used ultrasound to record variations in amplitude when scanning the human brain in 1937. This marked the first time that ultrasound was used in the medical setting and several advancements since then have created the modern ultrasound devices we use today.
Pioneers of modern lung ultrasound techniques
Although ultrasound had been integrated into almost every medical specialty by the 1990s, it had never been used to evaluate the lung. This was primarily because air in lung scatters ultrasound waves, resulting in artifacts that can be difficult to interpret. However, in the late 1990s, Daniel Lichtenstein, who is often referred to as the “father of lung ultrasound,” published a landmark paper describing the interpretation of lung ultrasound artifacts to detect lung pathology.
How lung artifacts changed the game
Lichtenstein’s work dramatically transformed the diagnostic and therapeutic landscape of lung ultrasound. Continued innovation and research demonstrated that artifacts called B lines correlated with thickening in the spaces between lung units - a condition now known as “interstitial syndrome.” Furthermore, Lichtenstein recognized that airless (ie. consolidated) lungs could be easily visualized with lung ultrasound.
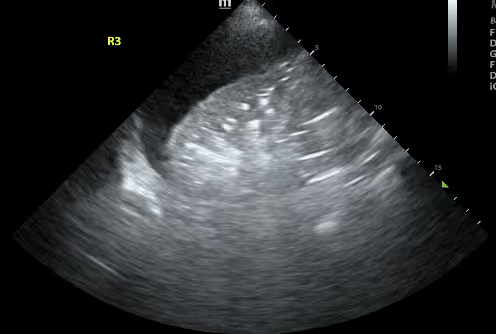
The development of portable ultrasound devices
Early users of point-of-care ultrasound (POCUS) often struggled with large and complex ultrasound machines. Fortunately, technological advancements led to creation of portable ultrasound devices that are easily used at the bedside. In recent years, handheld ultrasound devices have become the fastest-growing segment in the ultrasound market since they are much more cost-effective and portable than laptop and cart-based systems.

Integration into clinical practice
While initially used by intensivists to assess critically ill patients, lung POCUS is now used in almost every specialty - from Trauma teams who use it to rapidly diagnose pneumothorax, hemothorax and lung contusions to Radiologists and Internists who use it to identify safe needle insertion sites for drainage of pleural effusions. In the Emergency Department and Intensive care unit, lung POCUS has been shown to expedite diagnosis and reduce the number of imaging studies.
Ongoing research and future prospects
Despite its widespread use, there is a limited pool of well-trained physicians who are able to successfully teach and apply the use of lung POCUS in everyday practice. Furthermore, given that lung POCUS relies on the interpretation of artifacts, it is susceptible to subjectivity and limited reproducibility. Thus, current research centers around integrating artificial intelligence (AI) algorithms to guide the acquisition and analysis of lung ultrasound data. This advancement holds the potential to enhance the objectivity and reproducibility of pattern analysis, marking a turning point in evolution of lung ultrasound technology.
Here at Deep Breathe, our technology seamlessly merges the functionality of lung ultrasound with deep learning algorithms. Our goal is to replicate expert clinician interpretation of lung ultrasound so that individuals who do not have training in the use of lung ultrasound can expertly diagnose and manage pulmonary pathology. Check out some of our work here: Deep Breathe AI | Products


Arazi, O. (2023, January 30). Ultrasound Technology’s origins and evolution-and where it’s headed next. Forbes. https://www.forbes.com/sites/forbestechcouncil/2023/01/27/ultrasound-technologys-origins-and-evolution-and-where-its-headed-next/?sh=549dc1b44ba7
De Rosa, L., L’Abbate, S., Kusmic, C., & Faita, F. (2022). Applications of artificial intelligence in lung ultrasound: Review of Deep Learning Methods for covid-19 fighting. Artificial Intelligence in Medical Imaging, 3(2), 42–54. https://www.wjgnet.com/2644-3260/full/v3/i2/42.htm
Duck, F. A., & Thomas, A. (2022). Paul Langevin (1872-1946): The father of ultrasonics. Medical Physics, 10(1). http://mpijournal.org/pdf/2022-01/MPI-2022-01-p084.pdf
Lichteinstein, D., Meziere, G., Biderman, P., Gepner, A., & Barre, O. (1997). The comet-tail artifact. American Journal of Respiratory and Critical Care Medicine, 156(5), 1640–1646. https://www.atsjournals.org/doi/10.1164/ajrccm.156.5.96-07096
Newman, P. G., & Rozycki, G. S. (1998). The history of Ultrasound. Surgical Clinics of North America, 78(2), 179–195. https://www.sciencedirect.com/science/article/abs/pii/S003961090570308X?via%3Dihub
Soni, N. J., Arntfield, R., & Kory, P. (2020). Point of care ultrasound. Elsevier. https://shop.elsevier.com/books/point-of-care-ultrasound/soni/978-0-323-54470-2