B lines on lung ultrasound point to a variety of disease processes that extend beyond just heart failure. We explore the diagnostic criteria, differential diagnosis and clinical integration of B lines.

SHARE
TABLE OF CONTENTS
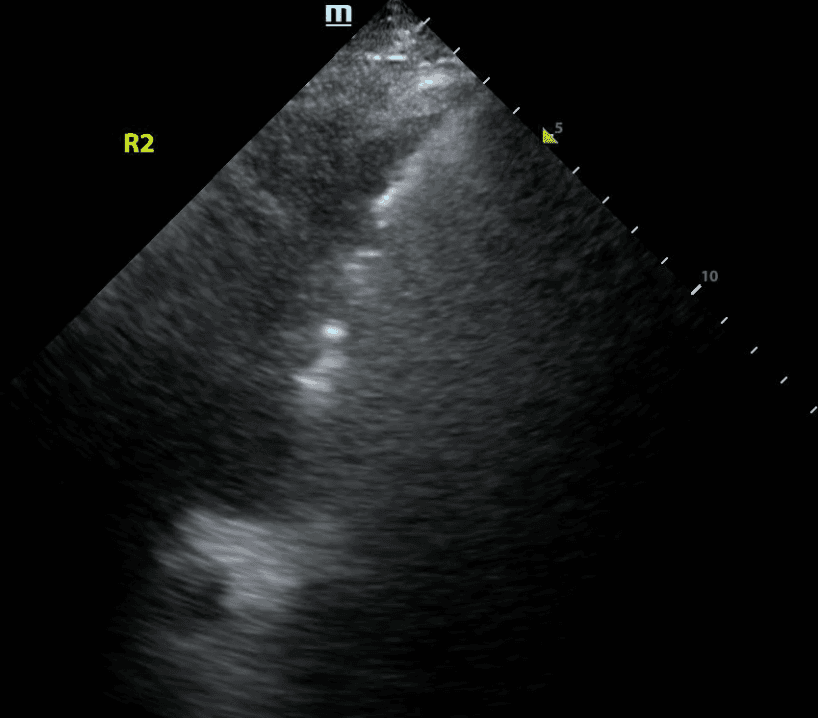
Recall that B lines are vertical hyperechoic artifacts originating from the pleural line that look similar to comet-tails.
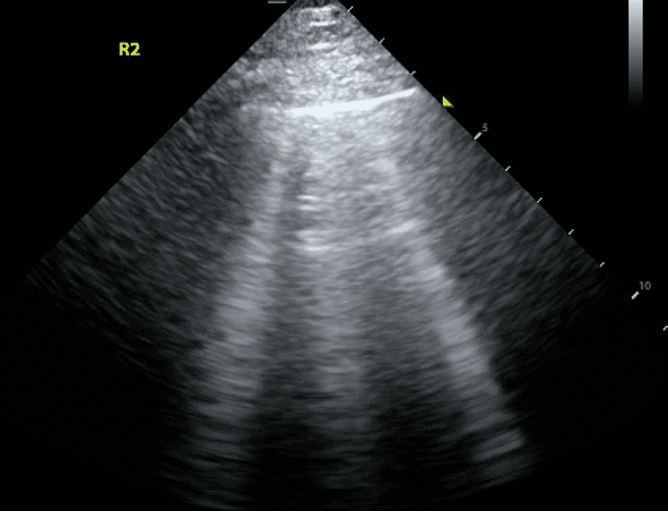
B lines are NOT present in a pneumothorax. This is because B lines only occur at the interface between the pleura and the tissue. Thus, if B lines are present at a specific location, we can say that with certainty, there is no pneumothorax.
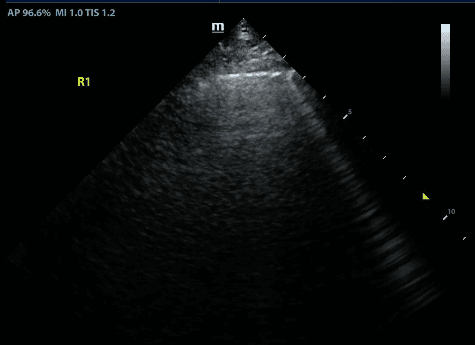
B lines at the lung bases are common due to gravity pulling physiologic lung fluid downward. Thus, occasional B lines at the lung bases do not usually signify pathology but if excessive or coupled with other abnormal features, can give a clue to underlying lung disease.
B lines reflect interstitial syndrome and the number of B lines increase with decreasing air content in lungs and thus, increasing lung density. To narrow down this broad differential, one can evaluate whether the B lines are present in a diffuse or focal (clumped together) pattern, look at abnormal pleural line patterns and look for other features of abnormal lung on ultrasound.
It is important to consider whether B lines are present in one or both lungs. Bilateral B lines are present in conditions that affect the lung diffusely. Two classic examples are cardiogenic pulmonary edema and acute respiratory distress syndrome (ARDS). In contrast, unilateral B-lines suggest a more localized process such as pneumonia, pulmonary contusion or neoplasia.
Pleural line abnormalities are another relevant marker in diagnosis lung disease. A normal pleura is thin and smooth. A thick or irregular pleural line is usually due to inflammatory conditions, such as pneumonia. However, the pleura in non-inflammatory diseases, like congestive heart failure, is often smooth and thin.
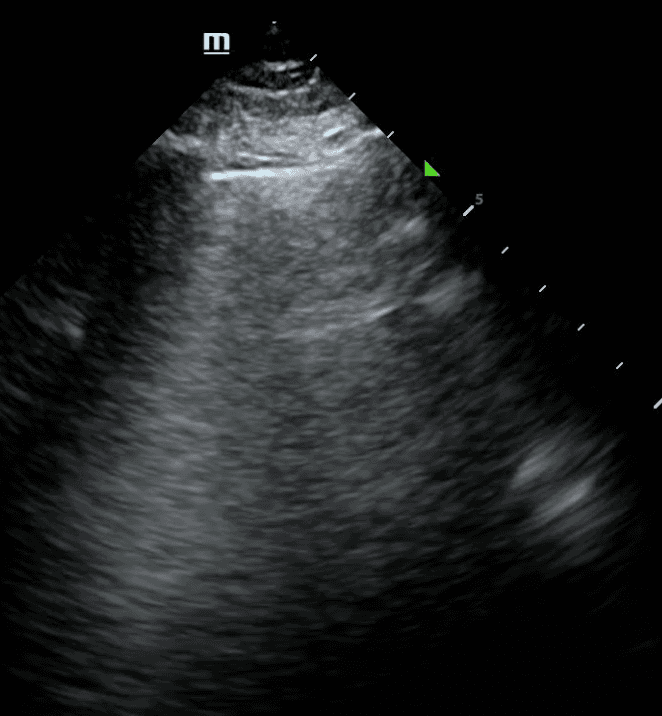
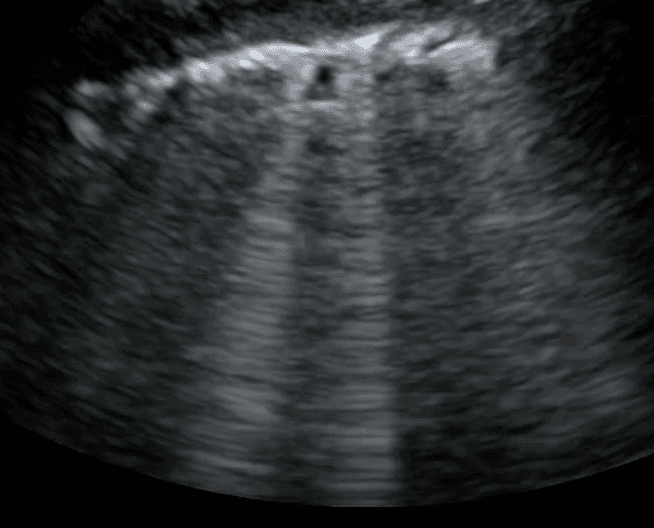
Other lung ultrasound features such as subpleural consolidation, shred sign and dynamic air bronchograms can point to inflammatory conditions including pneumonia or ARDS. One of the earliest lung ultrasound findings of pneumonia is that of localized B lines with small areas of subpleural consolidation due to loss of air-filled lung. Learn more about consolidations here.
A branch point for the differential diagnosis of B lines includes cardiogenic versus noncardiogenic causes. Integrating lung and cardiac ultrasound can be helpful, as left ventricular dysfunction or valvular heart disease with diffuse, bilateral B lines is highly indicative of cardiogenic pulmonary edema. In these cases, B lines can be monitored daily in order to guide optimal diuretic dosing. In contrast, diffuse, bilateral B lines with a normal heart ultrasound points toward a noncardiogenic cause of pulmonary edema, including ARDS or multifocal pneumonia.
Similar to other imaging modalities, it is of utmost importance integrate B line findings with the patient’s clinical context. B lines themselves are inherently a non-specific finding. For this reason, they should be assessed alongside the patient’s history, clinical presentation, lab values and other ultrasound findings described above to greatly improve diagnostic specificity. Establishing the correct diagnosis for interstitial lung syndrome is key as conditions such as heart failure and pneumonia have very different management plans.
In conclusion, the presence of B lines can rule out a pneumothorax and can narrow down the broad differential diagnosis of dyspnea. Their location, pattern, quantity and association with artifacts including pleural abnormalities, subpleural consolidation, shred sign, dynamic air bronchograms and cardiac findings can differentiate between many acute care pathologies with high specificity in real-time. This dynamic and radiation-free bedside imaging can allow for faster and more specific diagnosis and treatment than traditional chest radiography.
References
Bhoil R, Ahluwalia A, Chopra R, Surya M, Bhoil S. Signs and lines in lung ultrasound. J Ultrason. 2021 Aug 16;21(86):e225-e233. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8439137/
Biswas, A., Lascano, J. E., Mehta, H. J., & Faruqi, I. (2017). The utility of the “shred sign” in the diagnosis of acute respiratory distress syndrome resulting from multifocal pneumonia. American Journal of Respiratory and Critical Care Medicine, 195(2), e20–e22. https://www.atsjournals.org/doi/10.1164/rccm.201608-1671IM?url_ver=Z39.88-2003&rfr_id=ori:rid:crossref.org&rfr_dat=cr_pub%20%200pubmed
Dietrich, C. F., Mathis, G., Cui, X.-W., Ignee, A., Hocke, M., & Hirche, T. O. (2015). Ultrasound of the pleurae and lungs. Ultrasound in Medicine & Biology, 41(2), 351–365. https://www.umbjournal.org/article/S0301-5629(14)00670-X/fulltext
Gargani, L. (2011). Lung ultrasound: a new tool for the cardiologist. Cardiovascular Ultrasound, 9, 1–9. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3059291/
Lee, F. C. Y. (2016). Lung ultrasound—a primary survey of the acutely dyspneic patient. Journal of Intensive Care, 4(1), 1–13. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5007698/
Marini, T. J., Rubens, D. J., Zhao, Y. T., Weis, J., O’Connor, T. P., Novak, W. H., & Kaproth-Joslin, K. A. (2021). Lung ultrasound: the essentials. Radiology: Cardiothoracic Imaging, 3(2), e200564. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8098095/
Mojoli, F., Bouhemad, B., Mongodi, S., & Lichtenstein, D. (2019). Lung ultrasound for critically ill patients. American Journal of Respiratory and Critical Care Medicine, 199(6), 701–714. https://www.atsjournals.org/doi/10.1164/rccm.201802-0236CI?url_ver=Z39.88-2003&rfr_id=ori:rid:crossref.org&rfr_dat=cr_pub%20%200pubmed
Murali, A., Prakash, A., Dixit, R., Juneja, M., & Kumar, N. (2022). Lung ultrasound for evaluation of dyspnea: a pictorial review. Acute and Critical Care, 37(4), 502–515. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9732207/
Rippey, J. (2022). Lung Ultrasound: Pneumonia. Life in the Fastlane. https://litfl.com/lung-ultrasound-pneumonia/
Soldati, G., & Demi, M. (2017). The use of lung ultrasound images for the differential diagnosis of pulmonary and cardiac interstitial pathology. Journal of Ultrasound, 20, 91–96. https://pubmed.ncbi.nlm.nih.gov/28592998/
Vial, M. R., & Grosu, H. B. (2017). Practice pearls for performing pleural ultrasound with focus on pleural effusion and pleural thickening. US Respiratory & Pulmonary Diseases, 12, 23–25. https://www.touchrespiratory.com/wp-content/uploads/sites/11/2017/12/private_articles_22325_pdf_US-RESP-2.1_23-5_0.pdf
von Groote-Bidlingmaier, F., & Koegelenberg, C. F. N. (2012). A practical guide to transthoracic ultrasound. Breathe, 9(2), 133–142. https://breathe.ersjournals.com/content/breathe/9/2/132.full.pdf
SHARE
© 2025, DEEP BREATHE, INC