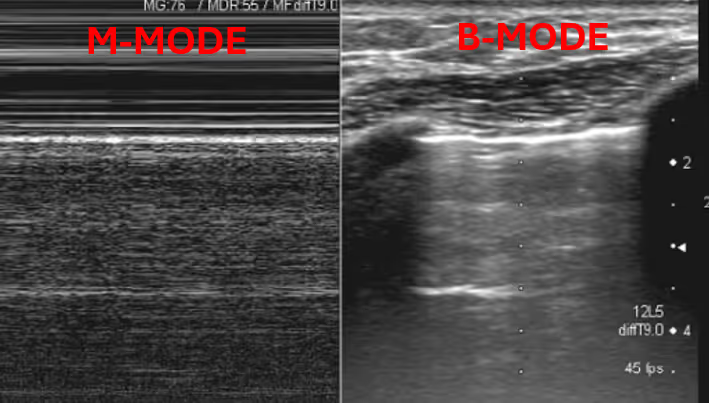
Nursing Led Lung Ultrasound
In recent years nurses have shown growing comfort with the application of ultrasound technology in areas such as IV placement (read more here). As point of care ultrasound continues to transform the landscape of healthcare, we must also imagine how this frontier will advance nursing practice.
Situational awareness
In many scenarios nurses are found at the bedside with a deteriorating patient in a busy hospital where delays in acquiring diagnostic tests delay treatment of potentially life-threatening respiratory conditions. If nurses were trained in point of care ultrasound, they could evaluate real time data that would substantially reduce time to diagnosis and appropriate treatment. Let’s imagine a few examples across the hospital where nursing led lung ultrasound would be beneficial.
New admission to the ICU
A sick patient arrives in the ICU and a central line was recently placed. Suddenly, the patient’s oxygen levels drop and they develop hypotension. The nurse is worried about pneumothorax - a life-threatening diagnosis where the lung collapses. The patient is too sick at this point to go down for an x-ray and there is only one portable x-ray technologist available in the hospital at this time of night.
However, with bedside ultrasound, the nurse could accurately rule out pneumothorax and assess for other dangerous conditions of the lung.
A night shift on a busy surgical unit
It’s 2 am in a busy thoracic surgery unit when the call bell goes off. When the bedside nurse comes to the room, they find their patient is sitting at the side of the bed struggling to catch their breath. Their vital signs show that they have an abnormal heart rate and low oxygen levels. The doctor has gone home for the night and when called, orders a chest x-ray to rule out pleural effusion - a dangerous accumulation of fluid in the chest cavity that may require immediate drainage.
Unfortunately, the portable x-ray technologist is busy with another patient. With bedside lung ultrasound, the nurse could rapidly identify pleural effusion with high accuracy and facilitate treatment.

The rapid response team
The rapid response team nurse receives a call for a septic patient who has a low blood pressure. The patient has already received one liter of IV fluid but given the patient’s history of heart failure, the team is hesitant to give further fluids. The patient is not requiring oxygen and does not appear to have any trouble breathing. The nurse orders a portable chest x-ray to check for signs of fluid in the lungs.
With bedside ultrasound, the nurse could quickly identify if the patient had B-lines - a sign that is pathognomonic for fluid in the lungs. In the absence of B-lines, the team would feel more comfortable giving IV fluids to address the patient’s low blood pressure.
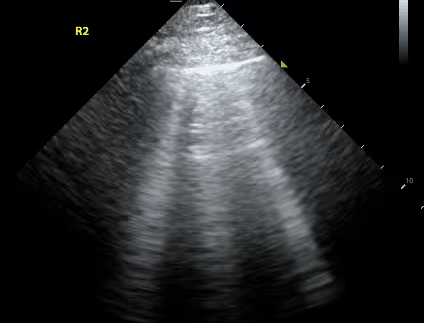
In practice today
Several institutions have realized the potential benefit of nursing led point-of-care ultrasound and have already begun implementing this into nursing practice. Kalam et al studied nurses who received standardized training in lung ultrasound and inferior vena cava (IVC) scans on septic patients in the emergency department. They were then asked to make recommendations on fluid management. Emergency physicians agreed with nursing ultrasound assessments in 99.1% of cases. Nursing ultrasound images changed management or increased physician confidence in current treatment plans 83.7% and 96.6% of the time respectively. A prospective, observational study conducted at a mixed medical and surgical academic ICU assessed the effectiveness of nurse led thoracic ultrasound. This study found that twenty-seven (27%) of ultrasounds led to a change of management and of all management changes, those most often executed were within the nursing scope of practice (56%).
Nursing comfort
The nursing profession is an ever-evolving field. In the last several years, different challenges in health care delivery have led nurses to adapt and develop new skills to accommodate their patients’ needs. This includes the implementation of ultrasound technology. A study showed that 62% of nurses were interested in learning and using lung ultrasound to rule out pneumothorax. Nurses that were more experienced or more comfortable with technology were more likely to feel comfortable performing a scan and interpreting it themselves.
Conclusion
The exploration of nursing led lung ultrasound is well underway and there is robust evidence to support nursing ultrasound. At Deep Breathe, we aim to accelerate this transition by integrating artificial intelligence (AI) into lung ultrasound technology to assist non-ultrasound experts in its acquisition and interpratation.

Douglas, T., Levine, A., Olivieri, P., McCurdy, M., Papali, A., Zubrow, M., Rodick, K., Hurley, J., Verceles, A. (2019) Brief training increases nurses’ comfort using tele-ultrasound: A feasibility study. Intensive and Critical Care Nursing. 51, 45-49. https://linkinghub.elsevier.com/retrieve/pii/S0964-3397(18)30103-4
Sullivan, R., Hutchinson, C., Baston, C. (2019) Nursing perceptions of a nurse-driven point-of-care ultrasound evaluation to rule out pneumothorax following lung biopsy. CHEST. https://journal.chestnet.org/article/S0012-3692(19)32360-8/fulltext
Geer, B. (2021) Using point of care ultrasound in nursing. Nursing. 51(6), 50 – 52. https://journals.lww.com/nursing/abstract/2021/06000/using_point_of_care_ultrasound_in_nursing.14.aspx
Kalam, S., Selden, N., Haycock, K., Lowe, T., Skaggs, H., Ding, V. (2023) Evaluating the effects of nursing-performed point-of-care ultrasound on septic emergency department patients. Cureus 15(6). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10350309/
Meissner, V. (2022) The Use of Lung Ultrasound for Detection of Fluid Overload in Patients on Dialysis and Its Applicability to Routine Nursing Practice: A Literature Review. Nephrology Nursing Journal. 49(5). https://pubmed.ncbi.nlm.nih.gov/36332125/
Smits, T., Heldeweg, M., Tullenken, A., Verlaan, B., Floor, L., Eijsenga, A., Lust, E., Gelissen, H., Girbes, A., Elbers, P., Tuinman, P. Effects of nurse delivered thoracic ultrasound on management of adult intensive care unit patients: A prospective observational study. International Journal of Nursing Studies Advances. 5, 100135. https://www.sciencedirect.com/science/article/pii/S2666142X2300019X